Lab-grown ovarian ‘mini-tumours’ provide new tool for immunotherapy research
Researchers at Barts Cancer Institute (BCI), Queen Mary University of London, have developed a way to grow miniature ovarian tumours in the lab that mimic the tumour environment found in patients.
The new approach offers a useful way to study how cancer cells interact with the immune system and to explore potential treatments. Ultimately, it could help accelerate progress for patients and reduce reliance on research methods involving animals.
The study, led by Professor Fran Balkwill and Dr Beatrice Malacrida, is published today (25th March) in Nature Communications.
Ovarian cancer remains one of the most difficult cancers to treat. Around 7,500 women are diagnosed each year in the UK, but only around 50% of those with the most common type – high-grade serous ovarian cancer (HGSOC) – survive beyond 5 years.
One of the challenges in studying this disease is the complex community of cells that surrounds the tumour, known as the tumour microenvironment.
“Cancers are not just malignant cells – they shape and are shaped by other cells in their environment. Understanding the tumour microenvironment is absolutely critical to understanding how cancers work and how to treat them,” explains Professor Fran Balkwill, Group Leader and Director of Research at Barts Cancer Institute. “Our model is a step forward towards studying cancer more realistically in the lab. Ultimately, better models will allow us to generate answers more quickly and drive progress for patients sooner.”
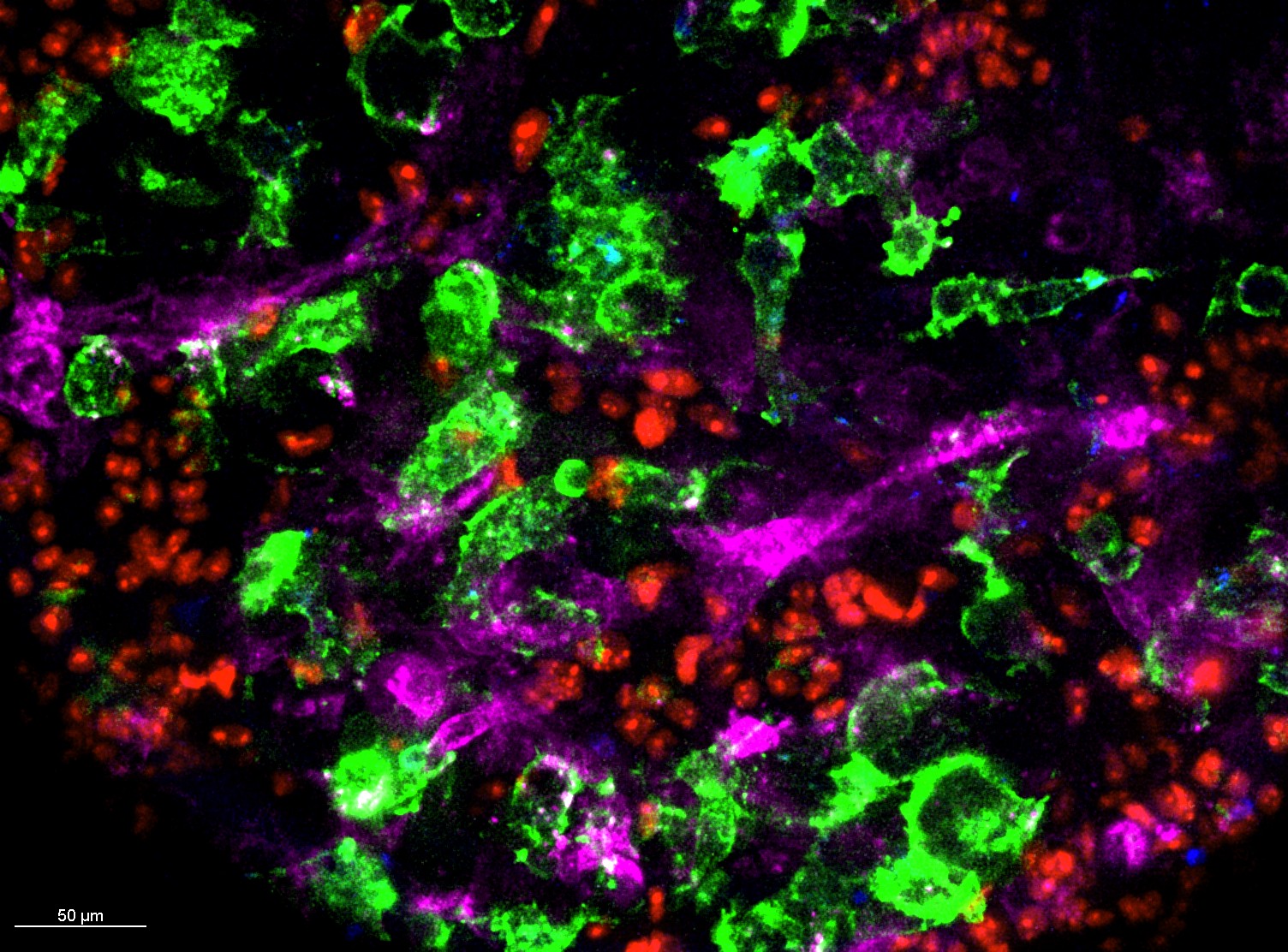
The team created a system called a pentaculture that combines five types of human cells commonly found in ovarian tumours and surrounding tissues: ovarian cancer cells, fat cells, organ lining cells, structural support cells, and a type of immune cell called monocytes. These cells organise into a 3D structure that mirrors human tumours.
“We wanted to build a lab model of a tumour that comes as close as possible to replicating the complexity we see in people with cancer,” says lead author Dr Beatrice Malacrida, a postdoctoral researcher in Professor Balkwill’s team.
Understanding how tumours shape immune responses
The researchers examined how immune cells act within their model. Similarly to real human tumours, they found that the monocytes developed into macrophages – specialised immune cells that can engulf cancer cells and play an important role in either supporting or limiting tumour growth. The macrophages behaved differently depending on which ovarian cancer cells they were grown with, highlighting how differences between tumours may influence how the immune system responds.
Macrophages are attracting growing interest as targets for new cancer immunotherapies designed to help them recognise and remove cancer cells. The team’s model offers a useful tool for studying and testing these approaches.
The researchers used the model to investigate treatments designed to block ‘do not eat me’ signals that cancer cells use to avoid being removed by macrophages. When they blocked these signals using antibodies, macrophage activity increased and cancer cell numbers decreased.
Using live microscopy, the team was also able to observe macrophages interacting with and engulfing tumour cells in real time.
These findings demonstrate how the pentaculture model can be used to explore potential treatment strategies and better understand how tumours influence immune responses.

Supporting new approaches to cancer research
The technique could also provide a valuable alternative to some research methods involving animals and may offer more relevant insights because it is based on human cells.
This supports wider efforts, including a commitment recently announced by the UK Government, to phase out animal research in favour of alternative methods, where appropriate.
“This model captures more of the human tumour environment than we’ve been able to study before. It allows us to think about what we can do using human cells, without always relying on research in animals such as mice,” Professor Balkwill comments. “However, it is still a simplified system, and there are important aspects of the tumour microenvironment we can’t yet fully replicate.”
The researchers note that in future, their model could be expanded to include additional cell types, enabling the study of even more complex tumour environments.
The study was made possible through collaboration with gynaecological oncology surgeons at Barts Health NHS Trust, led by Professor Ranjit Manchanda, who provided human tumour samples for the research. The team was also supported by core facilities at BCI, including pathology, microscopy and flow cytometry.
The work was funded by UK Research and Innovation (under the UK Government’s Horizon Europe funding guarantee), Cancer Research UK, the Ovarian Cancer Research Alliance, Wellbeing of Women, and Barts Charity.
Category: General News, Publications
No comments yet