New £1m clinical trial launches to improve quality of life for people with blood cancer
Dr Kevin Rouault-Pierre and team at Barts Cancer Institute, Queen Mary University of London, have been awarded funding to launch a new clinical trial aiming to improve quality of life for people living with a form of blood cancer called myelodysplastic syndromes, which currently has limited treatment options.
The new £1m grant from Cancer Research UK will fund a partnership led by Dr Rouault-Pierre at Barts Cancer Institute and Dr Onima Chowdhury at the MRC Weatherall Institute of Molecular Medicine and Oxford University Hospitals, working with Birmingham Clinical Trials Unit.
The study, which is based on a previous discovery by Dr Rouault-Pierre and his team, will test whether a high-dose of vitamin B5 can help reduce severe anaemia in patients with myelodysplastic syndromes carrying a mutation in the gene SF3B1.
This phase II clinical trial will take place across multiple sites in the UK, bringing together researchers and clinicians to translate the previous laboratory findings into a potential new treatment approach.
Addressing an unmet need
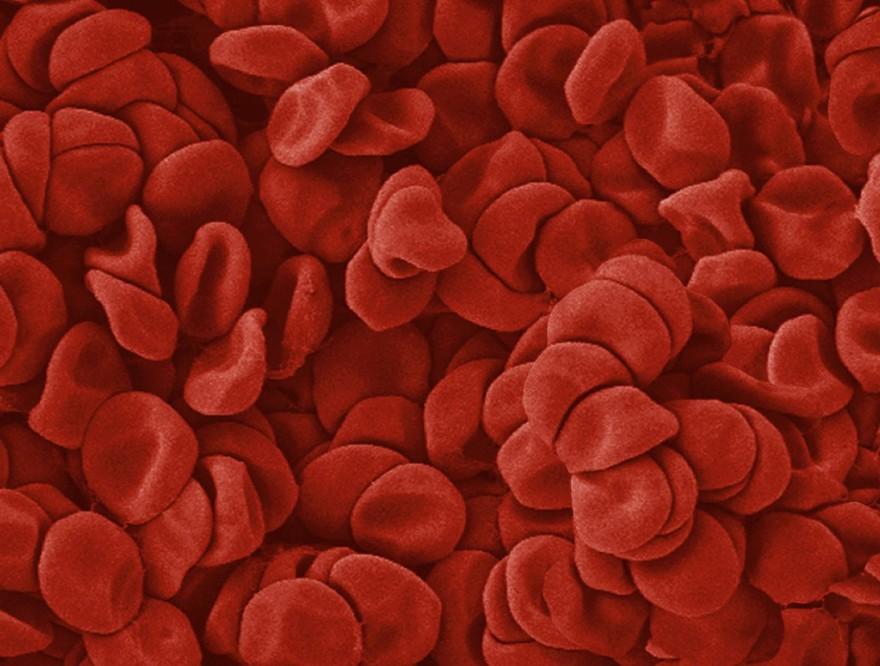
Myelodysplastic syndromes are a group of blood disorders in which the production of healthy red blood cells goes wrong. These patients often develop persistent and severe anaemia, requiring blood transfusions (typically every few weeks) for the rest of their lives.
While transfusions can help manage symptoms, they can also lead to complications such as iron overload in the blood and place a substantial burden on patients’ daily lives. Many older adults with the disease are not eligible for stem cell transplants, and around half of people become resistant to existing treatments for MDS within 18 months to two years of treatment.
“This group of patients currently has very few options,” explains Dr Rouault-Pierre. “Our aim is to offer an alternative approach that will reduce the burden of anaemia and improve day-to-day life using a treatment that is simple and well tolerated.”
From laboratory discovery to clinical trial
The trial builds on previous research from Dr Rouault-Pierre’s lab, published in Science Translational Medicine. The team found that mutations in the gene SF3B1 – the most common genetic change associated with the disease – led to a defect in an enzyme called COASY, which is crucial for healthy red blood cell development. However, they showed that administering vitamin B5 could circumvent this problem and help restore normal red blood cell production in stem cells isolated from people with this mutation.
Since then, the team has worked to translate these findings into a clinical setting, establishing collaborations with clinical partners and working closely with patients through the MDS UK patient support group to shape the study.
The five-year study will recruit around 30 patients with myelodysplastic syndromes who carry a mutation in SF3B1. The trial will take place in seven sites across the UK, including centres in Birmingham, Oxford, London, Manchester and Scotland.

Participants will receive high doses of vitamin B5 taken orally each day over a 24-week period. The researchers will assess whether the treatment increases haemoglobin levels, a key indicator of red blood cell production and will monitor how the treatment affects patients’ need for transfusions.
The study will also provide important information about how the body processes vitamin B5 at these doses, an area where data is currently limited. Blood and bone marrow samples collected during the trial will be analysed at Barts Cancer Institute, helping researchers better understand how patients respond to the treatment.
Looking ahead
If the trial shows promising results, the team hopes to expand the study internationally and explore whether the approach could benefit a wider group of patients with MDS. There is also potential to investigate how it might work alongside other treatments used outside the UK.
For now, the focus is on establishing whether this simple, low-toxicity approach can make a meaningful difference for patients.
“We want to see whether this can reduce the need for transfusions and give people more independence in their daily lives,” says Dr Rouault-Pierre. “If successful, this could open the door to a more accessible treatment option for patients who currently have very few choices.”
Read more
Category: General News, Publications
No comments yet